Introduction
Surgical Site Infections (SSIs) are among the most common healthcare-associated infections worldwide. They cause preventable patient suffering, extend hospital stays, and place billions of dollars of pressure on healthcare systems.
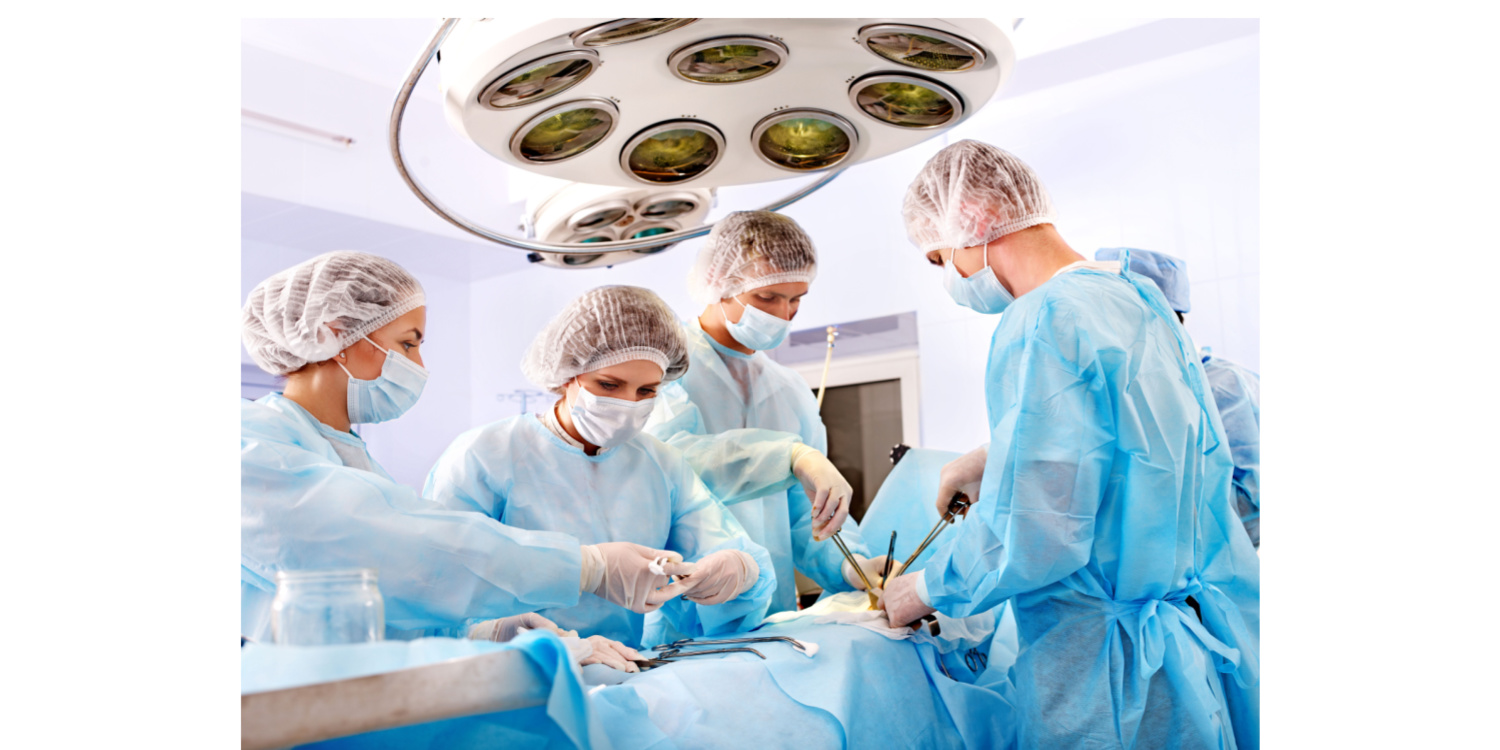
Across Australia, the USA, the UK, and Canada, the numbers tell the same story: SSIs remain costly and impactful. Yet, it is important to acknowledge that perioperative professionals — operating room nurses, surgical technologists, and Operating Department Practitioners (ODPs) — are already doing their best in highly complex environments.
The opportunity lies not in asking individuals to “do more,” but in creating collaborative systems and workflows that allow best practices to be followed seamlessly, every time.
The Global Burden of SSI
-
Australia: Around 16,500 SSIs annually in public hospitals, costing A$323 million in direct care and up to A$2.9 billion in broader indirect costs. Each infection adds about 20 extra hospital days costing approximately A$18,814, per case.
-
United States: SSIs account for 20% of all healthcare-associated infections, costing the system US$3.3 billion annually. Each infection adds ~9–10 extra hospital days and US$20,000–25,000 per admission .
-
United Kingdom: Risk varies by surgery — 0.5% in hip replacements, up to 19.9% in biliary procedures. On average, 5% of surgical patients experience SSIs. The cost of treating a wound infection ranges from £2,500–£4,900, with NHS England recording nearly 40,000 SSI cases annually .
-
Canada: SSIs occur in 2–5% of surgeries, with an average cost of CAD $28,000 per case and 7–11 additional hospital days. Surveillance shows SSI rates are improving in some specialties, but the burden remains high .
The Human Impact
For patients, an SSI is more than a complication. It means longer recovery, repeat surgeries, lost income, and sometimes life-threatening sepsis. Families bear emotional and financial strain, while healthcare staff experience frustration when complications could have been prevented.
Behind every statistic is a patient who deserved better.
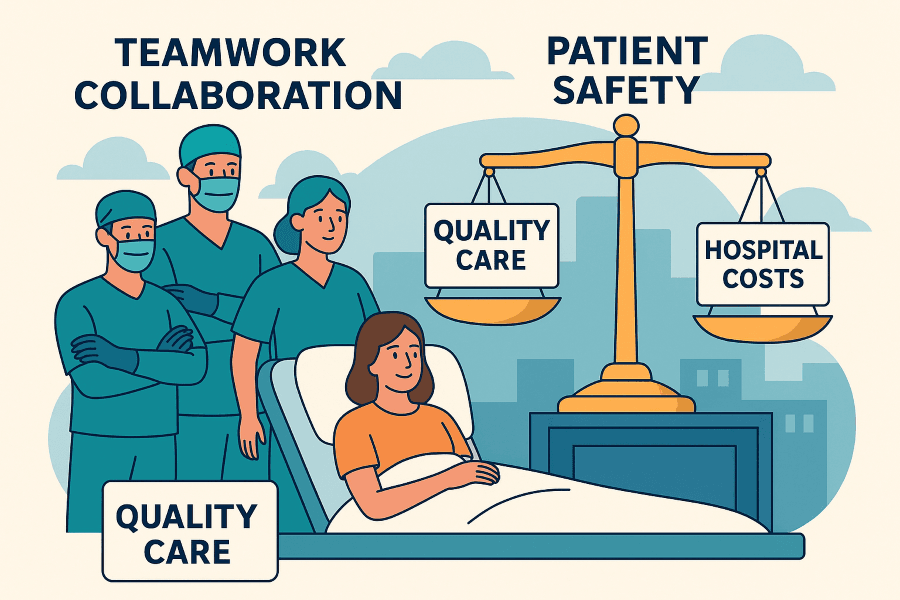
The Role of Perioperative Professionals Are Aligned
👩⚕️ Operating Room Nurses
-
Safeguard the sterile field and ensure aseptic handling.
-
Advocate for patients by confirming antibiotics, prep, and environmental readiness.
-
Monitor surgical counts and documentation that prevent error and infection.
🔧 Surgical Technologists (Scrub Techs)
-
Handle sterile instruments, sutures, and implants with precision.
-
Anticipate contamination risks and act quickly to address them.
-
Model best practice during critical moments under surgical pressure.
🎓 Operating Department Practitioners (ODPs)
-
Support both anaesthetic and scrub teams to maintain safety at every phase.
-
Ensure antibiotics, warming, and oxygenation protocols align with guidelines.
-
Act as communication bridges across disciplines, enhancing teamwork.
From Individual Vigilance to Team-Based Prevention
Perioperative teams are already vigilant. The real challenge is ensuring that systems support them to succeed.
-
Collaboration, not silos: Every team member — nurse, ODP, tech, anaesthetist, surgeon — must share accountability for infection prevention.
-
Seamless best practice integration: SSI bundles (antibiotic timing, antisepsis, normothermia, glucose control) should be built into workflows so they don’t feel like “extra tasks.”
-
Culture of speaking up: Hierarchy must never block action. Every voice in the OR matters when safety is at stake.
-
Continuous learning: Regular audits, debriefs, and education ensure evolving practices are embedded without adding stress.
Conclusion: A Shared Responsibility
Operating room professionals already give 100% to every patient, every day. The way forward is not to expect more from individuals but to enable teams to work more collaboratively, with systems and processes that make the safest practices and the easiest to follow.
By embedding best practices seamlessly into workflows, empowering all voices, and reinforcing teamwork, we can significantly reduce surgical site infections.
Together, through collaboration and by supporting quality assurance to maintain clinical standards, we can protect patients, strengthen surgical teams, and ease the financial and emotional burden of SSIs worldwide.
📑 References
- Royle R., Gillespie B. M., Chaboyer W., et al. The burden of surgical site infections in Australia: A cost-of-illness study. Journal of Infection and Public Health, 2023. (2018–19). https://www.sciencedirect.com/science/article/pii/S1876034123000989
-
CDC. National Healthcare Safety Network (NHSN) Patient Safety Component Manual: Surgical Site Infection (SSI) Event. 2025. CDC SSI Manual PDF
-
Anderson DJ, et al. Strategies to Prevent Surgical Site Infections in Acute Care Hospitals. Infection Control & Hospital Epidemiology, 2022.https://pubmed.ncbi.nlm.nih.gov/37137483/
- Guest J.F., Fuller G.W., Griffiths B. Cohort study to characterise surgical site infections after open surgery in the UK’s NHS. BMJ Open. 2023;13:e076735. https://pmc.ncbi.nlm.nih.gov/articles/PMC10748996/
-
Jenks PJ, et al. Clinical and economic burden of surgical site infection (SSI) and prediction of risk. BMJ Open, 2014;4:e003765.https://pubmed.ncbi.nlm.nih.gov/24268456/
-
PHAC (Public Health Agency of Canada). Device and surgical procedure–related infections in Canadian hospitals, 2011–2020. Canada Communicable Disease Report (CCDR), 2022. https://pmc.ncbi.nlm.nih.gov/articles/PMC10278973/
-
CPSBC & ORNAC. Surgical Site Infection Surveillance and Standards in Canada. College of Physicians and Surgeons of BC / ORNAC, 2020. https://www.cpsbc.ca/files/pdf/NHMSFAP-AS-Environmental-Cleaning-Operating-Procedure-Rooms-and-Sterile-Core.pdf
- StatPearls. Postoperative Wound Infections. SSIs affect ~0.5%–3% of inpatient surgeries. https://www.ncbi.nlm.nih.gov/books/NBK560533/#:~:text=Approximately%200.5%25%20to%203%25%20of,develop%20a%20surgical%20site%20infection.
- Rezaei, A. R., Zienkiewicz, D., & Rezaei, A. R. (2025). Surgical site infections: A comprehensive review. Journal of Trauma and Injury, 38(2), 71–81.https://doi.org/10.20408/jti.2025.0019