The Hidden Cost of Losing Operating Room Expertise
Posted at 12 May 2026 in Clinical Education,Clinical Governance,Clinical Quality & Safety,Healthcare Education,Healthcare Leadership,Operating Room,Operating Room Education,Patient Safety,Perioperative Nursing,Staff Wellbeing by Marrianne
Why perioperative workforce retention is becoming one of healthcare’s greatest global challenges 🛡️
Experience Matters in the Operating Room
Behind every safe surgical procedure is a highly skilled perioperative team balancing patient safety, workflow coordination, communication, anticipation, technology, and critical decision-making in real time.
Yet globally, operating rooms are approaching a major workforce transition.
The World Health Organization estimates a projected global shortage of approximately 4.5 million nurses by 2030, with workforce gaps continuing to impact healthcare systems worldwide.
Within perioperative care, the challenge is even more complex.
Perioperative nursing is one of the most specialised areas of healthcare. It requires years of procedural exposure, situational awareness, technical skill, communication, anticipation, adaptability, and hands-on clinical experience developed within real operating room environments.
Unlike many other clinical areas, perioperative clinicians must continuously coordinate multiple moving parts simultaneously:
⚕️patient safety
🩺sterile technique
🔄surgical workflow
🧠instrumentation
💻technology integration
⚙️equipment troubleshooting
⏳emergency response
🤝communication between multidisciplinary teams
📋procedural anticipation under pressure
These are not skills learned overnight.
Research highlights that it may take 6–12 months for a perioperative nurse to achieve proficiency, with training and orientation costs estimated between $80,000–$88,000 AUD per nurse. Australian workforce studies have also estimated average nursing turnover costs of approximately $49,255 AUD per full-time nurse, with specialty workforce losses significantly higher due to orientation, productivity reduction, temporary staffing, and lost expertise.
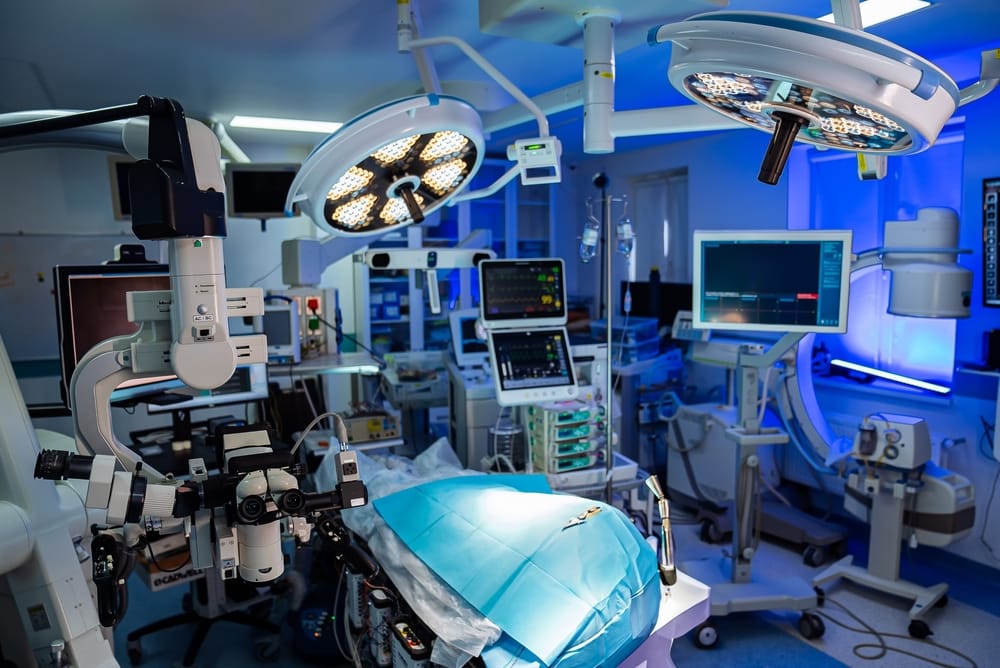
But perhaps the greatest cost is the one least measured:
The Loss of Experience
Every experienced perioperative nurse, surgical technologist, ODP, anaesthetic nurse, technician, or operating room support professional who leaves healthcare takes with them years of accumulated procedural knowledge, pattern recognition, workflow intelligence, communication ability, equipment familiarity, troubleshooting capability, and patient safety expertise that cannot simply be replaced by orientation alone.
Experienced perioperative teams contribute far beyond task completion.
They:
🧠identify risk early
🛡️anticipate surgeon needs before requests are verbalised
🩺recognise subtle patient deterioration
✅coordinate teams during emergencies
🎯troubleshoot equipment failures rapidly
🧠maintain sterile workflow under pressure
🛡️mentor junior clinicians
🩺reduce procedural delays
✅improve communication and theatre efficiency
💙strengthen safety culture within operating rooms
Research continues to show that insufficient staffing and burnout contribute to workflow disruption, increased stress, reduced team stability, cancelled surgeries, adverse patient outcomes, and growing pressure on remaining clinicians.
This is no longer simply a staffing issue.
It is:
- a patient safety issue
- a healthcare sustainability issue
- a workforce resilience issue
- an operational efficiency issue
- a clinical governance issue
The Future of Surgical Care

Technology must support the humans delivering care
The future of surgical care will not depend solely on advancing technology.
It will depend on how well we:
🧠 preserve knowledge
🤝strengthen mentorship
💙support workforce wellbeing
🛡️improve retention
💰invest in perioperative education
🛡️create psychologically safe workplaces
⚕️support clinicians at the point of care
Technology should not replace clinical experience.
It should help preserve, support, and strengthen it for the next generation of perioperative professionals.
Because when we support perioperative teams, we support patients.
References
- World Health Organization. Nursing and Midwifery Fact Sheet. World Health Organization. Available at: https://www.who.int/news-room/fact-sheets/detail/nursing-and-midwifery
- Xie A, et al. Perioperative Nursing Shortages: An Integrative Review of Contributing Factors, Impacts, and Strategies. 2024.
- Roche M, et al. Nursing Workforce Turnover and Associated Costs in Australia.
- Li Y, et al. Understanding Burnout Among Operating Room Nurses. 2025.
Recent Articles
Electrosurgery & Cautery Safety: Protecting Patients Through Vigilance, Communication, and Best Practice
09 December 2025
✈️From Pilots to Perioperative Practice: Why Organisation and Readiness Save Lives in the OR
28 October 2025
Categories
More articles from Clinical Education,Clinical Governance,Clinical Quality & Safety,Healthcare Education,Healthcare Leadership,Operating Room,Operating Room Education,Patient Safety,Perioperative Nursing,Staff Wellbeing
View AllElectrosurgery & Cautery Safety: Protecting Patients Through Vigilance, Communication, and Best Practice
⭐ A Personal Note on Perioperative Practice Every day in the operating room, perioperative professionals carry a...
09 December 2025
Read more✈️From Pilots to Perioperative Practice: Why Organisation and Readiness Save Lives in the OR
Instrument nurses anticipate, troubleshoot, and act quickly under the direction of the surgeon and surgical team. T...
28 October 2025
Read moreWhy Interruptions in the Operating Room Put Safety, Efficiency, and Staff Wellbeing at Risk
The Hidden Cost of Interruptions in the OR: Why Focus Matters Imagine this: mid-operation, a circulator is execu...
26 September 2025
Read more